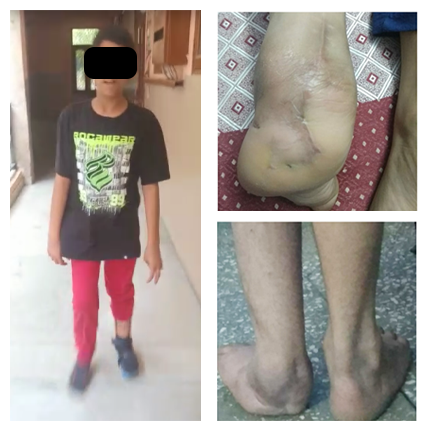
Musculoskeletal infections in children are considered orthopaedic emergencies. Because a child’s immune system and bone structure (specifically the blood supply near growth plates) are unique, infections can spread rapidly and cause permanent damage if not treated within hours or days.
1. Types of Infections
There are two primary categories of musculoskeletal infections in children:
- Osteomyelitis (Bone Infection): Infection within the bone itself. It usually starts in the "metaphysis" (the area right next to the growth plate) because the blood flow there is slow, allowing bacteria to settle.
- Septic Arthritis (Joint Infection): Infection within a joint space (most commonly the hip or knee). This is more urgent than osteomyelitis because the bacteria can destroy joint cartilage in as little as 8 to 24 hours.
2.Common Causes
- Bacteria: Staphylococcus aureus (Staph) is the most common culprit. In recent years, MRSA (methicillin-resistant Staph) has become more frequent and aggressive.
- Route of Infection: In children, bacteria usually reach the bone or joint through the bloodstream (hematogenous spread) from a minor cut, a sore throat, or an ear infection. It can also occur directly through a deep puncture wound.
3. Signs & Symptoms
Parents should look for the "Red Flags":
- Refusal to Bear Weight: A child who suddenly stops walking or starts limping.
- Pseudoparalysis: An infant who stops moving one specific arm or leg (it looks paralyzed, but it is actually just too painful to move).
- Fever and Irritability: Often accompanied by localized warmth, redness, and swelling.
- Pain with Motion: In septic arthritis, any attempt to move the joint—even gently—causes extreme pain.
4. Diagnosis: The "Workup"
Doctors use a combination of tests to confirm an infection:
- Blood Tests: * WBC (White Blood Cell Count): Often elevated.
- CRP (C-Reactive Protein) & ESR (Sed Rate): These measure inflammation levels. CRP is especially useful because it rises and falls quickly, helping doctors track if treatment is working.
- Imaging: * X-rays: Often look normal in the first few days of an infection. Ultrasound: Used to look for fluid (pus) inside a joint.
- MRI: The "gold standard" for spotting bone infections early.
- Joint Aspiration: Using a needle to take a sample of fluid from the joint to "culture" it and identify the specific bacteria.
5. Treatment Principles
The goal is to "wash out" the bacteria and kill the remaining germs with medicine.
Treatment
- Surgical Drainage: For joint infections (Septic Arthritis) and many bone abscesses, surgery is required to wash out the pus and debris to save the cartilage.
- Antibiotics:Initially given through an IV. Once the infection is under control, the child may transition to high-dose oral antibiotics for 3 to 6 weeks.
- Splinting:The affected limb is often immobilized in a splint to reduce pain and protect the bone while it heals.
6. Potential Complications
If treatment is delayed, the consequences can be life-altering:
- Growth Plate Damage: Resulting in a limb that is shorter or crooked.
- Chronic Osteomyelitis: A long-term infection that is very difficult to clear.
- Joint Destruction: Leading to early, severe arthritis and loss of mobility.
Note: If your child has a fever and refuses to walk or move a limb, do not wait. Seek evaluation in an Emergency Room immediately.
Case - 1
Before
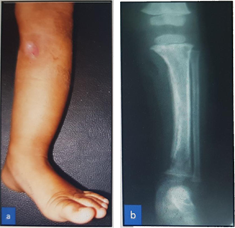
After
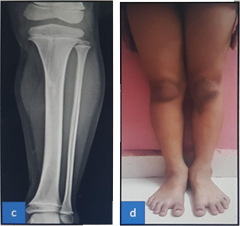
Case - 2
Before
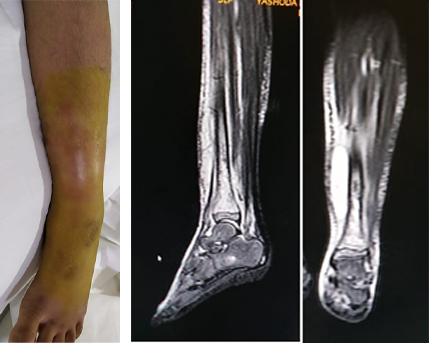
Pre Operative clinical image showing significant swelling and redness & MRI showing intraosseous, subperiosteal and subcutaneous collection.
After
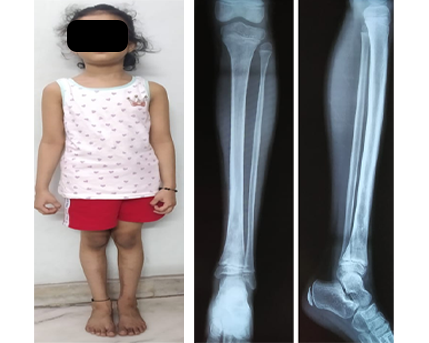
6 month follow up clinical image and X rays showing no leg length descripancy and healed wound.
Case - 3
Before
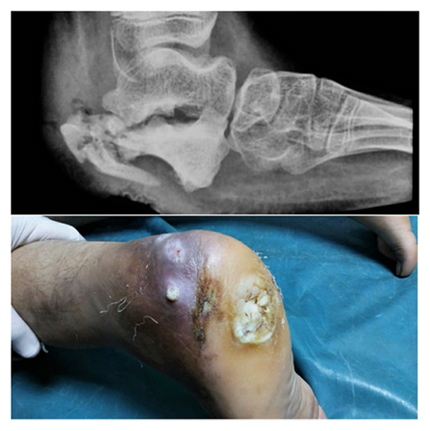
Figure showing X ray and clinical image of Chronic osteomyelitis left heal with non healing ulcer post meningomyelocoele
After